Most examples of biomimicry I am familiar with are from the world of medical devices. As discussed in class today, implants and prosthetics mimic the anatomical part or physiologic function they replace.
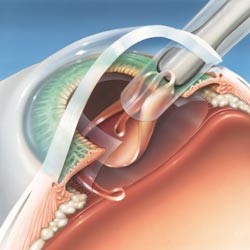
HIGHLIGHT: Example of a successful biomimetic implant – Intraocular Lens (IOL)
Problem statement: Most people, if they live long enough, will develop a clouding of the eye’s natural lens. This phenomenon, known as cataract, historically led to blindness in most cases (and in some parts of the world still does). Lens removal surgery restores basic visual function, but leaves the patient with a debilitating degree of myopia, requiring extremely thick glasses for correction.
Biomimetic solution: A small plastic implant can mimic the eye’s natural lens and restore near perfect vision (at least for distance vision). Today’s intraocular lens (IOL) implants are based on a 1949 invention by British ophthalmologist Harold Ridley. Modern-day IOLs are inserted into the eye through a micro-incision and can correct vision at several distances, mimicking the natural process of accommodation. With about 10 million cases per year, cataract surgery is one of the most frequent surgical interventions worldwide.
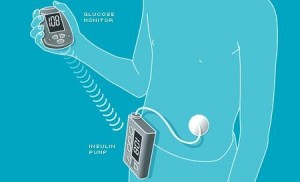
LOWLIGHT: Example of an (as of yet) unsuccessful biomimetic concept – Insulin Pump
Problem statement: Diabetes is a wide-spread (and growing) disease caused by an insulin insufficiency. In the case of Type 1 diabetes (and some Type 2 cases), the therapy of choice is insulin replacement: Patients inject themselves regularly with synthetic human insulin, which mimics the function of the body’s own insulin production. The issue in many elderly patients is a lack of compliance with the therapy, which has to be followed consistently to be effective.
Biomimetic solution: Insulin pumps attempt to mimic the natural “dosing algorithm” of the pancreas more closely than a series of manual injections can. In particular they mimic the so-called basal rate of near-constant insulin production in a healthy pancreas between meals. Insulin pumps were described as early as the 1960, but generally Dean Kamen (who later invented the Segway) is credited with creating the first wearer-friendly version in 1976. In my view as a Type 1 diabetic, insulin pumps do not solve the actual user problem. They are costly, bulky, still require manual input and periodic replacement of the subcutaneous needle. The degree of mimicry achievable with conventional therapy is arguably the same. Only a fraction of Type 1 diabetics actually use a pump.